

Arterial Blood Gas (ABG) Interpretation Made Easy: A Step-by-Step Guide Medical Students and Healthcare Professionals
Learn arterial blood gas (ABG) interpretation step by step with normal values, clinical examples, and common mistakes explained for medical students and healthcare professionals.
Interpreting arterial blood gas (ABG) results is one of the most challenging yet essential clinical skills for medical students and healthcare professionals. Many learners struggle to connect ABG numbers with real clinical decision-making. This guide explains ABG analysis step by step, combining normal values, interpretation logic, and practical clinical examples to help you confidently interpret ABGs in exams and real patient care. This article is especially designed for medical, nursing, and health sciences students seeking a clear and practical approach to ABG interpretation.
ABG analysis is a key diagnostic tool and the gold standard that measures oxygen (PaO₂), carbon dioxide (PaCO₂), and pH in the blood. It helps assess oxygenation, ventilation, and acid-base balance, which is crucial in managing respiratory, circulatory, and metabolic disorders. ¹
ABGs are more accurate than non-invasive methods like pulse oximetry or end-tidal CO₂ and are widely used in emergency, ICU, anaesthesiology, and pulmonology settings. ¹
Clinical Importance and Indications of Arterial Blood Gas (ABG) Analysis
Clinically, ABG analysis plays a central role in evaluating and managing the following conditions:
- Respiratory failure (acute or chronic)
- ARDS, sepsis, or shock
- Diabetic ketoacidosis and renal tubular acidosis
- Heart failure, cardiac arrest, and asthma
- Inborn errors of metabolism
Serum bicarbonate (HCO₃⁻) is usually calculated from ABG values, and small differences may exist between calculated and measured values, especially in critically ill patients. ¹
Technical Challenges and Clinical Examples
Arterial blood sampling is a crucial procedure for critical care physicians. Since Stephan Hales first cannulated the arterial and venous vessels of a horse in 1711, the technique has evolved and remains essential in the management of critically ill patients. Measuring arterial pH, oxygen (PaO₂), and carbon dioxide (PaCO₂) provides accurate information on acid-base balance and gas exchange. While many critically ill patients have an arterial catheter in place, it is important for medical trainees and intensivists to be proficient in arterial puncture, understand the procedure, and recognize its potential pitfalls. ³
- Technical Challenges
In patients with shock, obesity, or weak pulses, ultrasound-guided arterial puncture significantly improves success rates and reduces complications.
- Difficulty obtaining the sample in uncooperative patients or those with weak pulses (e.g., shock, vasopressor use, arteriosclerosis).
- Positioning difficulties: if the patient cannot fully extend the wrist or has joint contractures.
- Obesity or limb edema may obscure the artery.
- Solution: Use ultrasound to locate the artery and reduce complications from repeated punctures. ²
Clinical Examples Requiring Frequent ABG Monitoring:
- Shock: To assess lactic acidosis and respiratory compensation.
- COPD exacerbation: To assess acute respiratory failure (respiratory acidosis) and CO₂ retention.
Practical Steps for Obtaining an Arterial Blood Gas (ABG) Sample
1. Arterial Sampling Methods
Needle puncture:
- Blood is drawn directly via needle without placing a catheter.
- Suitable for patients needing few ABG tests (e.g., once daily).
- If more than 4 times in 24 hours, rotate sites or consider an indwelling arterial catheter. ²
Indwelling catheter:
- Requires written consent before insertion.
- Less painful if frequent blood draws are needed.
- Ultrasound use: Not routine but helpful if standard access is difficult (weak pulses, vasopressors, obesity). ²
2. Site Selection
Common sites: Radial (wrist), Brachial (arm), Femoral (groin), Axillary (armpit), Dorsalis pedis (foot).
Most used: Radial artery, because it is accessible and more comfortable. Other sites are suitable for inpatients depending on need. ²
3. Ensure Collateral Circulation
For small arteries (Radial, Dorsalis pedis), check that other arteries supply the area to prevent ischemia. ²
Common tests:
- Allen Test / Modified Allen Test: Hand clenched, both arteries compressed, then release one artery to check color return within <10 seconds. If color does not return quickly, choose an alternative site.
- Large arteries (Axillary, Femoral) usually do not need collateral testing because blood flow is adequate. ²
4. Equipment
- Local anesthetic like Lidocaine if needed. ²
- ABG kit includes Heparinized syringe, Needle, Protective needle cover, Ice bag to preserve the sample
5. Puncture Sites and Details
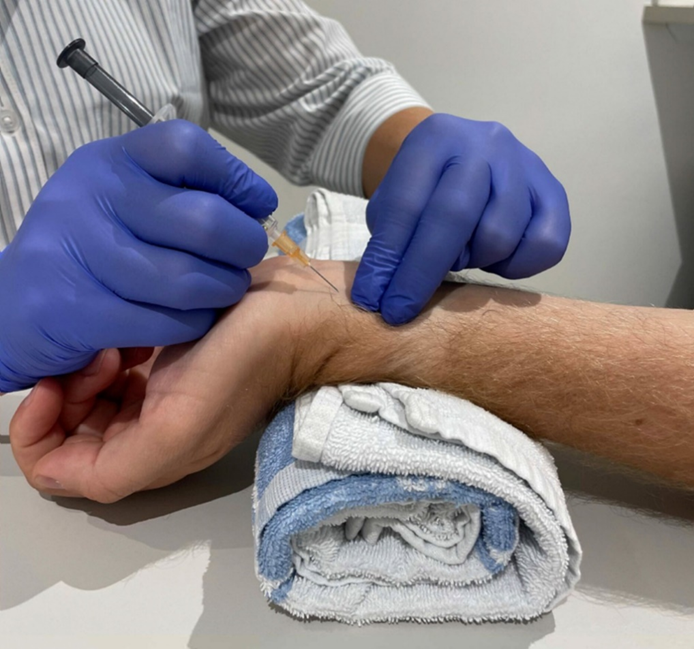
- Radial artery: Between the distal radius and flexor tendon. Patient’s hand extended, palm facing up. ²
- Brachial artery: Medial to biceps tendon. Needle inserted at 30° above the elbow crease.
- Femoral artery: Just below the midpoint of the inguinal ligament. Needle inserted at 90°. ²
- Axillary artery: In the armpit, arm abducted and externally rotated. Needle at the apex of the axilla.
- Dorsalis pedis: Dorsum of the foot, lateral to the great toe tendon. Needle inserted at 30°. ²
Normal Arterial Blood Gas (ABG) Reference Values
The following table summarizes the most commonly used normal ABG values and their clinical interpretation.
Interpretation | Normal range | Symbol | parameter |
| <7.35 = Acidemia; >7.45 = Alkalemia | 7.45-7.35 | pH | pH |
| >45 = Hypercapnia (Respiratory acidosis); <35 = Hypocapnia (Respiratory alkalosis) | 45-35 | PaCo2 | Partial pressure of carbon dioxide |
| <80 = Hypoxemia; >100 = Hyperoxemia. | 100-80 | Pao2 | Partial pressure of oxygen |
| <22 = Metabolic acidosis; >26 = Metabolic alkalosis. | 26-22 | HCO-3 | Bicarbonate |
| < -2 = Base deficit (Metabolic acidosis); > +2 = Base excess (Metabolic alkalosis). | -2 to +2 | BE | Base excess |
| <95% = Low oxygen saturation. | 100-95 | SaO2 | Oxygen saturation |
| >12 = High anion gap metabolic acidosis. | 12-8 | AG | Anion gap |
Note: Normal reference ranges may vary slightly between laboratories, altitude levels, and clinical conditions. ABG values should always be interpreted in clinical context.
How to Interpret Arterial Blood Gas (ABG) Results: A Step-by-Step Practical Guide
A structured approach to ABG interpretation helps avoid common mistakes and ensures accurate clinical decisions. Follow these steps sequentially for every ABG result.
Step 1: Assess the pH
- pH < 7.35 → Acidosis
- pH > 7.45 → Alkalosis
- Normal pH (7.35-7.45) → May indicate full compensation or a mixed disorder
Step 2: Identify the Primary Disorder
- Look at PaCO₂:
- If PaCO₂ is abnormal and changes in the opposite direction to pH → Disorder is Respiratory
- Example: Low pH (7.25) with High PaCO₂ (55) → Respiratory Acidosis
- Look at HCO₃⁻:
- If HCO₃⁻ is abnormal and changes in the same direction as pH → Disorder is Metabolic
- Example: Low pH (7.28) with Low HCO₃⁻ (18) → Metabolic Acidosis
Step 3: Assess the Compensation Mechanism
- Physiological compensation attempts to return pH toward normal
- Respiratory compensation for metabolic disorders:
- Metabolic acidosis → PaCO₂ decreases
- Metabolic alkalosis → PaCO₂ increases
- Metabolic compensation for respiratory disorders (takes 3-5 days):
- Chronic respiratory acidosis → HCO₃⁻ increases
- Chronic respiratory alkalosis → HCO₃⁻ decreases
Step 4: Calculate Anion Gap in Cases of Metabolic Acidosis
- Formula: Anion Gap = [Sodium] – ([Chloride] + [Bicarbonate])
- Normal: 8-12 mEq/L
- High anion gap (>12): Indicates presence of “unmeasured” acids (e.g., diabetic ketoacidosis, lactic acidosis)
- Normal anion gap: Indicates bicarbonate loss (e.g., severe diarrhea)
A normal pH does not always indicate a normal acid base state. Always consider the possibility of mixed disorders and assess compensation carefully.
Common ABG Interpretation Mistakes in Medical Students
Common mistakes include relying on pH alone, ignoring compensation mechanisms, misinterpreting normal pH in mixed disorders, and failing to calculate the anion gap in metabolic acidosis. Avoiding these errors improves both exam performance and clinical accuracy.
For example, a normal pH with abnormal PaCO₂ and HCO₃⁻ often indicates a mixed acid–base disorder rather than normal physiology.
Potential Complications
1. Sampling Complications:
- Hematoma, bleeding, infection
- Vasospasm, nerve injury (rare)
2. Complications Due to Misinterpretation:
- Delay in diagnosing and treating life-threatening conditions
- Inappropriate treatment based on incorrect results
3. Complications of the Disorders Themselves:
- Severe Acidosis: Cardiac arrhythmias, decreased response to inotropic drugs
- Severe Alkalosis: Cerebral vasospasm, seizures, hypokalaemia
Contraindications for Arterial Blood Gas Sampling
- Deficient collateral circulation to the distal extremity (especially for radial or dorsalis pedis sites). Can be assessed by Allen Test or alternative methods (Doppler, plethysmography, MRI).
- Overlying skin infection at the puncture site.
- Patients on anticoagulants or with coagulopathies – only if absolutely necessary due to increased bleeding/hematoma risk.
- Severe vascular disease or conditions making arterial access technically difficult (e.g., very weak pulses, severe arteriosclerosis).
Indications for Arterial Blood Gas Sampling
To obtain arterial blood for analysis of:
- Partial pressures of oxygen (PaO₂) and carbon dioxide (PaCO₂)
- Arterial pH
- Useful for assessing patients with acute or severe respiratory distress.
- Provides accurate information on acid–base balance and gas exchange.
- To perform CO-oximetry for detecting methemoglobinemia or carboxyhemoglobinemia.
- May guide ventilation and oxygen therapy decisions in critically ill patients. ⁴
Frequently Asked Questions (FAQ) About Arterial Blood Gas (ABG) Analysis
What does arterial blood gas (ABG) analysis tell us about a patient’s condition?
Arterial blood gas analysis helps us understand how well the lungs are working, how much oxygen is reaching the blood, and whether the body’s acid–base balance is normal. This makes it an important test for assessing a patient’s overall respiratory and metabolic status.
Conclusion
ABG analysis remains a vital diagnostic tool in clinical practice, especially in managing critically ill patients. The combination of correct sampling technique and systematic, accurate interpretation of results is key to maximizing the utility of this test. ABG results should always be interpreted within the context of the patient’s complete clinical picture, not in isolation from other examinations and clinical information. This chapter has covered vascular anatomy, indications, procedural steps, common complications, and interpretation challenges associated with arterial blood gas sampling. ³
Want to move from memorizing ABG values to truly understanding them?
Our step-by-step ABG course includes:
- Real ICU and ER cases
- Interactive ABG interpretation exercises
- Common exam traps and clinical pitfalls
👉 Start learning ABG interpretation the right way https://medskai.com
References
- https://www.statpearls.com/point-of-care/17837
- https://laemeufba.wordpress.com/wp-content/uploads/2016/07/4-arterial-blood-gases.pdf
- https://link.springer.com/chapter/10.1007/978-981-96-1202-4_15
- https://saude.ufpr.br/labsim/wp-content/uploads/sites/23/2019/01/Gasometria-NEJM.pdf
By /Esraa Hasaneen Mohamed
Categories
Archives
Tags
You May Also Like
-
-
April 19, 2026
-
-
April 8, 2026
-
-
March 27, 2026


















